The medical landscape of 2026 is defined by a remarkable intersection of biological advancement, clinical expertise, and human selflessness.
Few areas exemplify this intersection as powerfully as living liver donation—a procedure that is both a triumph of modern medicine and an extraordinary act of human devotion.
Unlike most organ transplants, which rely on the unfortunate occurrence of brain death or severe trauma, living liver donation is a proactive, intentional choice.
It is a decision made out of love, duty, or ethical commitment—a conscious act of giving a part of oneself to save another life.
For families facing the urgent realities of chronic liver disease, living donation represents a bridge over the unpredictable and often prolonged wait for a deceased-donor organ, offering a timely and life-saving solution.
The Biology of Regeneration
At the heart of living liver donation lies one of the human body’s most remarkable abilities: hepatic regeneration.
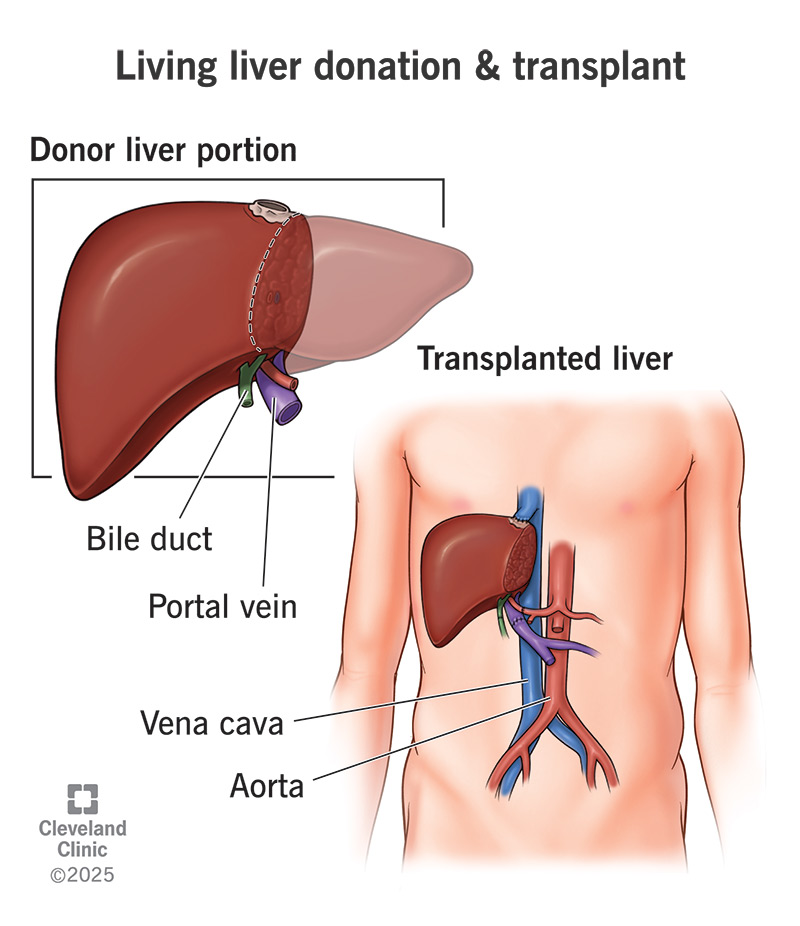
The liver is unique among internal organs in its capacity to restore both structure and function after surgical removal.
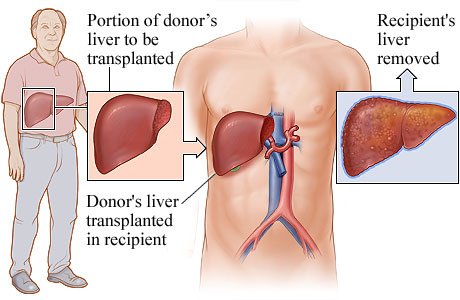
When a healthy adult undergoes living donation, a portion of the liver—commonly between 40 and 60 percent—is surgically excised and transplanted into a recipient whose liver is failing.
The remaining liver in the donor regenerates over the course of several weeks to months, returning to near its original size and functionality. The transplanted portion similarly regenerates within the recipient.
This regenerative capability is not just biological trivia; it is what enables living donation to exist as a safe and effective option. For older adults whose liver function may be deteriorating rapidly, waiting for a deceased donor can be a matter of life or death.
Living donation allows families to take an active role in the survival of their loved ones, reducing mortality risk and improving long-term outcomes.
The surgery requires an extraordinary level of precision, coordination, and expertise. Advances in imaging, minimally invasive surgical tools, and perioperative care have significantly reduced complications over the past decade.
Preoperative CT and MRI scans allow surgeons to map the donor’s vascular and biliary anatomy with incredible accuracy, ensuring compatibility and minimizing surgical risk. In 2026, leading transplant centers have implemented enhanced recovery pathways that reduce hospital stay and accelerate return to normal activity for donors, while still maintaining rigorous safety standards.

Intergenerational Sacrifice: A Family-Centered Narrative
Living liver donation is often framed as an intergenerational act of courage and devotion. Most commonly, adult children step forward to donate a portion of their liver to a parent.
Consider a scenario in which a son discovers that his father has end-stage liver disease, perhaps complicated by cirrhosis from hepatitis C, non-alcoholic fatty liver disease, or autoimmune hepatitis.
The father’s condition may be deteriorating rapidly, with standard liver function tests indicating high bilirubin, persistent ascites, and early signs of hepatic encephalopathy. In such cases, a timely transplant is the only option for survival.
The decision to donate is never taken lightly. Donors undergo weeks of comprehensive evaluation, including physical assessment, psychological screening, blood tests, liver imaging, and compatibility checks.
This process ensures that the donor is physically capable of tolerating the surgery and psychologically prepared for the emotional and social consequences of donation. Independent donor advocates are assigned to protect the donor’s interests, ensuring the decision is fully informed and voluntary.
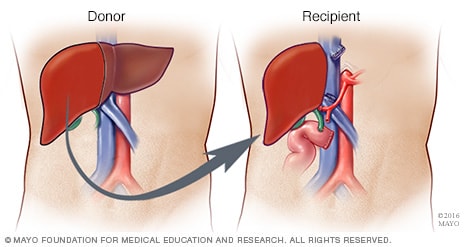
Once cleared, the surgical procedure is an intricate choreography. Both donor and recipient are brought into adjacent operating theaters. In what is known as “tandem surgery,” the liver segment is removed from the donor and immediately transplanted into the recipient.
This minimizes the time the liver is outside the body, which is critical for graft function. Surgeons work simultaneously on donor and recipient, sometimes with multiple surgical teams, to ensure efficiency and safety. The transplanted liver, being freshly sourced from a living, healthy individual, often demonstrates faster integration, better function, and lower risk of complications than organs from deceased donors.

The Recovery Journey: Realities and Challenges
While the outcome of living liver donation can be life-saving, the road to recovery is significant. Donors are hospitalized for approximately five to seven days following surgery, where they are closely monitored for complications such as bleeding, bile leaks, infections, or fluid accumulation. Pain management, early mobilization, and nutritional support are critical during this phase.
Once discharged, the donor faces weeks of fatigue as the body prioritizes liver regeneration. The liver, although resilient, demands a high metabolic input for tissue restoration, leaving donors temporarily depleted.
Physical stamina gradually returns, but complete recovery—both physical and emotional—may take several months. Donors are advised to maintain a high-protein diet, moderate physical activity, and regular follow-up imaging to ensure the liver is regenerating properly.
Psychological recovery is equally important. Donors often experience a complex mix of pride, relief, anxiety, and vigilance. They may struggle with lingering fears about long-term health, or experience subtle post-operative stress as they adjust to temporary lifestyle limitations.
Peer support programs, counseling, and structured follow-up care are now recognized as essential components of post-donation management, reinforcing the idea that donor care extends far beyond the operating room.
Transformative Effects on Family Dynamics
Beyond the surgical success, living liver donation can reshape the emotional and relational fabric of families. The shared experience of illness and recovery often strengthens connections that may have weakened over time.
Siblings who were previously distant may find common ground in the hospital waiting room. Grandchildren witness a profound example of selflessness, gaining early insight into empathy, duty, and courage.
The recipient’s experience is transformative as well. Recovery from end-stage liver disease is often accompanied by renewed energy, improved cognition, and restored physical function.
Patients regain autonomy in daily life, and a sense of gratitude and purpose permeates the family dynamic. Family members frequently report a deeper appreciation for the fragility and resilience of human life.
Community support plays a complementary role. Digital networks, social media advocacy groups, and local community organizations offer resources ranging from meal delivery and childcare support to financial assistance for medications and follow-up visits.
In 2026, hospitals frequently partner with local nonprofits to provide structured volunteer programs that assist families during the critical first months post-surgery. While the act of surgery occurs between two individuals, the broader healing process is a communal one.
Ethical Considerations and Long-Term Wellbeing
Living liver donation presents profound ethical considerations, particularly when adult children are involved. Transplant centers in 2026 place a strong emphasis on autonomy, informed consent, and the psychological health of donors.
Comprehensive education sessions, independent advocacy, and mental health evaluations ensure donors are not coerced, implicitly or explicitly, into the decision.
Post-donation care includes both short-term monitoring and long-term surveillance. Liver function tests, imaging studies, and regular consultations assess structural regeneration, while psychosocial support monitors for anxiety, depression, or post-traumatic stress related to the procedure.
This dual focus ensures that the donor’s wellbeing is as central to the medical process as the recipient’s.
For the aging population, these stories highlight the importance of proactive conversations about organ health, medical wishes, and end-of-life planning. Living liver donation is not only a medical procedure; it is a cultural touchstone that prompts families to consider legacy, responsibility, and intergenerational bonds in tangible terms.
Advancements in Surgical Technique and Safety
In 2026, living liver transplantation benefits from decades of iterative advancement. Minimally invasive techniques, such as laparoscopic or robotic-assisted donor hepatectomy, reduce incision size, pain, and recovery time.
Surgeons now employ real-time imaging and computer-assisted modeling to map vascular and biliary structures, minimizing the risk of post-operative complications.
Anesthesia protocols have improved dramatically, decreasing intraoperative stress and supporting hemodynamic stability. Post-operative care incorporates enhanced recovery after surgery (ERAS) principles: early mobilization, optimized nutrition, multimodal pain management, and close monitoring of liver function. Collectively, these innovations have made living donation safer than ever while preserving the extraordinary regenerative promise of the liver.
Clinical Outcomes and Research
Data from transplant registries indicate that living liver donors have excellent long-term outcomes. Most donors return to normal activity levels within three to six months and maintain healthy liver function over decades. Complication rates are low, with severe adverse events occurring in less than 5 percent of cases.
Recipient outcomes are also favorable, with graft survival rates often surpassing those associated with deceased-donor organs due to the shorter ischemic time and superior organ quality.
Ongoing research continues to explore liver regeneration, post-operative recovery protocols, and long-term psychosocial outcomes. Studies in 2026 emphasize the importance of individualized care plans that account for age, comorbidities, and social support systems.
The integration of telemedicine and wearable monitoring devices allows transplant teams to track recovery more accurately, ensuring prompt intervention if complications arise.
Societal and Cultural Impact
The ripple effects of living liver donation extend far beyond the operating room. It serves as a tangible demonstration of human altruism and the power of science to amplify compassion. In a world characterized by political uncertainty, environmental stressors, and rapid technological change, these acts of medical selflessness provide hope and affirmation of shared humanity.
Media coverage, educational campaigns, and patient advocacy programs have increased public awareness of living donation. Cultural narratives increasingly celebrate the courage of donors and the resilience of recipients, highlighting not just the medical triumph, but the ethical and emotional significance of the procedure.
Social media platforms facilitate storytelling that normalizes organ donation and encourages discussions around health literacy, family planning, and preventive care.
Preparing for a Living Donation
For families considering living donation, preparation is multifaceted. Potential donors undergo rigorous medical evaluations including liver function panels, imaging studies, and assessments of cardiovascular health. Psychological readiness is assessed through counseling and structured interviews. Nutritional optimization, physical conditioning, and lifestyle adjustments are recommended to maximize safety and recovery outcomes.
Recipients also undergo extensive evaluation, including assessment of disease severity, comorbidities, and suitability for surgery. Pre-operative education covers lifestyle modifications, post-transplant immunosuppressive therapy, and potential complications.
This comprehensive approach ensures that both donor and recipient enter the process with realistic expectations and thorough understanding.
The Legacy of Living Donation
Living liver donation is not merely a medical intervention—it is a deeply human story of courage, compassion, and interconnection. It reminds us that the body, while biological, is also a vessel for ethical and emotional expression.
A father who regains health to witness the milestones of grandchildren, a son who discovers renewed purpose through his gift, or a family whose bonds are strengthened in the face of adversity—all reflect the profound societal and personal impact of this practice.
It is an enduring testament to human resilience and the possibilities of modern medicine. While risks remain and recovery is substantial, the act of living donation encapsulates hope, selflessness, and the remarkable regenerative power of the human body. In 2026, living liver donation continues to stand as one of the clearest examples of how science, compassion, and family converge to save lives and inspire generations.
